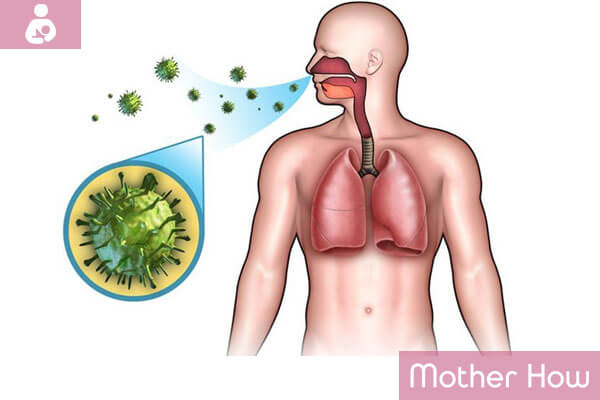
Diphtheria is an acute life-threatening infectious disease. It proceeds as an acute inflammation of the upper respiratory tract, predominantly the pharynx (about 90% of the cases). The inflammation of the nose, skin in the place where it is damaged, and the eyes or genitals are also frequently affected. However, the main threat is not inflammation but the poisoning with a toxin which is produced by bacterium (one that causes the disease) Predominantly cardiovascular and nervous systems are affected.
The Causative Agent of Diphtheria and Transmission Ways
The causative agent of diphtheria is Corynebacterium diphtheria. It is a Gram-positive bacteria in the form of rods with characteristic flask-shaped thickenings at the ends, which are arranged in pairs in smears, angled as Roman number V in relation to each other. Diphtheria bacilli produce diphtheria toxin, neuraminidase enzyme, and other biologically active compounds. The synthesis of diphtheria toxin by microbial cells is controlled by a special TOX gene.
Bacteria can lose it during life together with the ability to produce a toxin (toxigenicity). And vice versa, some initially non-toxigenic strains may acquire pathogenic properties. Fortunately, it is an extremely rare phenomenon. The disease is transmitted by airborne droplets from those who have diphtheria or from healthy carriers of the infection, less frequently – through household items.
Risk Group
The most susceptible to diphtheria infection is 3-7 years old, but the incidence among adolescents and adults has increased in recent years. The source of infection is sick people or healthy carriers of toxigenic bacteria. The highest infectious risk group refers to those suffering from the pharynx, nose, and throat diphtheria since they actively secrete pathogens through exhaled air. Those patients with eyes diphtheria, and skin diphtheria may transmit the infection through direct and indirect contact and touch (hands, household items).
Healthy carriers of bacteria are less contagious but due to the absence of any visible symptoms, it is difficult to control infection. Their illness may be diagnosed only in the case of mass dispensary surveys. As a result, most the cases of infection with diphtheria are caused by contacting healthy carriers of the diphtheria bacilli. The incubation period (time from infection until the first signs of the disease) is 2-10 days.
Diphtheria Toxin
The toxin, produced by diphtheria bacillus, consists of several components. One of them, the hyaluronidase enzyme, destroys hyaluronic acid increases capillary permeability and leads to coming out of the vessels and imbuing the surrounding tissues with blood plasma and fibrinogen deposition. The second component, a neurotoxin, destroys epithelium cells and the secretion of thrombokinase enzyme out of them takes place.
Thrombokinase promotes converting the fibrinogen into fibrin and the formation of a fibrin membrane on the surface of the tissues. The diphtheria toxin affects the palatine tonsils (which are covered by several layers of epithelium cells) and the fibroid membrane penetrating deep into the tonsillar epithelium and tightly welding to it.
The third (main) component – the toxin itself is able to block the process of cellular respiration and the synthesis of protein molecules. Among the most affected are the capillaries of myocardial cells and nerve cells. As a result, myocardial degeneration and infectious-toxic myocarditis may develop. The damaging of capillaries leads to infectious toxic shock. Damage to the Schwann cells (supporting cells of the nervous tissue) leads to demyelination of nerve fibers (destruction of the electrical insulation myelin level with a violation of nerve impulses along the nerve fibers). Furthermore, diphtheria toxin causes general intoxication.
Symptoms and Proceeding
Pharynx diphtheria usually begins with a small rise in body temperature, a minor pain when swallowing, redness, and swelling of the tonsils with the formation of specific membranous plaque on them. The increased front upper neck lymph node is also a symptom. Membranes are usually white during the first 2-to 3 days of the disease and later turn gray or yellow-gray.
The disease may be cured in about a week (a less severe form is observed in those who are vaccinated against diphtheria) or may become toxic due to the systemic effects of diphtheria toxin. The toxic form of diphtheria is always severe. It is characterized by a very high body temperature (39,5-41,0 ° C), severe headaches, drowsiness, and apathy. The skin becomes pale, the mouth becomes dry.

As for children the following symptoms reveal:
- Repeated vomiting and abdominal pain
- Edema tonsil becomes pronounced
- Complete closure of the entrance to the throat may appear
- The closure extends to the soft and hard palate, often also to the nasopharynx
- Difficult breathing, nasal voice often may occur
- Plaque applies to all tissues of the oropharynx
- A classic sign of a toxic form of pharynx diphtheria is swelling of the subcutaneous tissue in the neck and sometimes the chest, causing the skin to become jelly-like consistency
- Front upper neck lymph nodes are significantly enlarged and painful
- Diphtheria of the nose occurs with normal or slightly elevated body temperature, there is no intoxication
- Seropurulent or bloody purulent discharge from the nasal passages can be seen
- Soak and then dry crusts appear on the nose, cheeks, and forehead
- Membrane raids can be seen in the nose
- The pathological process can also affect the sinuses
- The swelling of neck and cheeks subcutaneous tissue may be observed in case of a toxic form of diphtheria
- Eye diphtheria proceeds as banal conjunctivitis and is characterized by mild hyperemia and edema of the eyelid, a small amount of serous-purulent conjunctival sac (catarrhal form)
- Membrane form is characterized by a pronounced swelling of the eyelids, the presence of the conjunctive of the white-gray The toxic form is also accompanied by swelling of tissue around the eye sockets
- Diphtheria of the skin leads to the long-term healing of any damage to the skin. Redness of the skin and presence of dirty-grey patina, as well as dense infiltration of surrounding skin, are typical in that case
Diagnosing
Diphtheria is diagnosed according to the examination of the infected person and the results of the analysis. It is characterized by typical membranes, difficult breathing, whistling sound during inhaling, and so-called barking coughing. If the less severe form takes place the diagnosing is very difficult.
Analyses
- General blood test for the signs of acute inflammation
- Smear examination under a microscope (bacterioscopy) – identification of the Corynebacterium diphtheria bacteria
- Bacteriological examination – inoculation of the biological material for a special growth medium and cultivating colonies of microorganisms
- Determination of the level (titer) of the antitoxin antibodies (titer higher – 0.05 IU / ml and above eliminates diphtheria)
- Serology – determination of serum-specific antibodies using methods HAI, ELISA, etc
Pharynx diphtheria should be differentiated from acute tonsillitis (follicular and lacunar form), Simonovsky – Vensan angina (fungal infection), syphilitic angina, pseudomembranous angina during infectious mononucleosis. It is also should be differentiated from a peritonsillar abscess, mumps, and leukemia. As for the children it should be differentiated from pseudo-croup.
Treatment
All patients with diphtheria should be hospitalized. The treatment includes:

- Dieting – vitaminized, calorie held thorough cooking of food.
- Causal treatment (ie, aimed at eliminating the causes of disease) – is the injection of diphtheria serum, the dose and the number of injections depend on the severity and form of the disease.
- Antibiotics: When milder forms – erythromycin, rifampicin inside, in moderate and severe forms – injections of penicillin or cephalosporin. Duration of the course – 10-14 days.
- Local treatment – rinsing and irrigation by disinfectant solutions.
- Detoxification Therapy – glucose-saline solutions, taking into account the daily requirement of fluid and its loss (moderate and severe).
- Corticosteroids – with moderate and severe forms.
- Bacillicarriers treatment with antibiotics: tetracycline (children older than 9 years), erythromycin, cephalosporin, in the purpose of strengthening therapy and eliminating chronic foci of infection.
Complications
Among the most serious complications of diphtheria on the cardiovascular system are:
- Myocarditis, cardiac arrhythmia
- Neurological complications of diphtheria are caused by lesions of various cranial and peripheral nerves and manifested by accommodation paralysis, strabismus, paresis of limbs, and in more severe cases paralysis of respiratory muscles and diaphragm muscles
- To secondary diphtheria complications, such pathological diseases as acute cerebral circulatory disorders (thrombosis, embolism), metabolic encephalopathy, cerebral edema, renal toxicity, diphtheria hepatitis, as well as toxic shock and disseminated intravascular coagulation (severe problems with blood clotting) should be attributed
- The toxic form of diphtheria can lead to acute renal, cardiovascular, respiratory, or poly-organ failure
- Peritonsillar abscess, otitis, and pneumonia are among the non-specific complications of diphtheria
Vaccination
Vaccination against diphtheria toxoid is performed with the help of inactivated toxin. Antibodies to the diphtheria toxin but not to Corynebacterium diphtheria are produced as the reaction. Traditionally the first vaccination is carried out before 18 months in combination with tetanus and pertussis (whooping cough) vaccines.
There are 4 known combinations of the vaccines – DTaP, Tdap, DT, and Td. The second vaccination is carried out between 4-7 years, and the third – is before 14. Adults must be re-vaccinated against tetanus and diphtheria every 10 years. In order to get the right vaccine at the right time, you should consult your doctor.

Born in Belarus, 1985, a pedagogue and family psychologist, mother. Taking part in procedures of social adaptation of the foster children in new families. Since 2015 is a chief editor of the motherhow.com project, selecting the best and up-to-date material for those, who are planning, expecting, and already having babies.

