Contraception (lat. «contraceptio» -. Liter. – exception) or birth control – the prevention of pregnancy by mechanical (condoms, cervical caps, etc.), chemical (eg, vaginal balls, spermacetical paste), and other contraceptive means and methods.
Some methods (eg, condoms, birth control patch) help to significantly reduce the risk of HIV and other sexually transmitted diseases.
In a few words, contraception is the means that prevent conception. Nature has provided all the mechanisms in order to keep the kind safe and sane. We choose partners according to the general principles that may guarantee the natural course of life: surviving and spreading your genes.
It is also provided that a woman has from 10 to 20 pregnancies during her fertility life. In the past times, that was normal. But due to the success of medicine, we are now able to preserve the weakest posterity of a human being and we can simply exclude the continuous delivery of new people. A 20 billion population on the planet is way too much. So the current conditions dictate the rule of 2 children in a family and just 1 for China.
Contraception has become an obligatory tool of birth control. But the natural mechanisms still work the same way and we experience true pleasure during sex. Women in particular, because nature had to justify the pregnancy, which has little to do with pleasure in the end.
Considering we are now having sex for fun, we still choose sex partners according to the natural configurations and behave differently during ovulation. That is where birth control kicks in states certain limits for our own natural cycles: we don’t get pregnant that often. And here comes the question: which way of contraception is the best and safest for our health?
“Barrier” Contraception
Barrier contraception – are male and female condoms, diaphragms, cervical caps. All these devices are physically overlapping the path of sperm into the uterus.

Condoms
We all know about male condoms, but the female ones are less popular. It’s a small bag, usually made of polyurethane, which is inserted into the vagina and fixed in by the elastic ring. The advantage of both types of condoms is that they not only prevent unwanted pregnancies but also protect against sexually transmitted infections.
The effectiveness of condoms is relatively high: according to the WHO, if used properly, male condoms prevent unwanted pregnancy in 98% of cases, but the women condoms – only in 90%. In addition, it is necessary to take into account that a condom can tear.
Caps
Vaginal diaphragm cervical cap – a latex cap of various shapes, which is put on the cervix. They do not protect the partners of gonorrhea or syphilis but do not let the sperm into the uterus. Their main disadvantage – the complexity of using (not every woman can wear the cap itself) and allergies that may occur due to the dense and prolonged contact with mucous latex.
“Natural” Contraception.
“Natural” refers to methods of protection, which do not require mechanical or pharmacological intervention.
Coitus Interruptus
One of the most popular and at the same time the least reliable “natural” methods. When using a partner remove his penis from the woman’s vagina a few moments before ejaculation. The unreliability of this method is determined by two factors. First, a man may not be able to remove his penis in time (it all depends on his ability to self-control). Second, during the frictions, a small amount of pre-cum liquid comes out, and it may contain some sperm and pathogenic agents. The effectiveness of the method, according to WHO, is from 73 to 96%, depending on proper use.
The Calendar Method
Another popular method, but not always effective. A woman keeps track of favorable and unfavorable days for conception during her menstrual cycle. A few days before ovulation (sperm can remain in the genital organs of women and wait for the mature egg) and a couple of days after ovulation are considered conception-friendly. Adherents of the calendar method claim that during this period the woman should abstain from sexual intercourse if she does not want to become pregnant. The disadvantage is that it’s not always possible to precisely calculate when exactly the ovulation occurs, especially for women with irregular cycles. You can know more about getting pregnant during your periods.
Temperature Method
This method allows you to specify the time of ovulation precisely. It is not for the lazy: every day just after waking up it’s necessary to measure the basal temperature (by inserting a thermometer into the anus). Before ovulation, basal temperature slightly decreases, and immediately after ovulation increases by 0.3-0.5 degrees, and lasts until the end of the cycle. By monitoring the temperature of the day, you can quite accurately determine when ovulation occurs, and in accordance with this refrain from intercourse during the favorable for conception days.
Cervical Method
Another method to determine the ovulation day is the cervical method or the Billings method. This Australian doctor noticed that shortly before ovulation, the mucus released from the vagina becomes more viscous. Thus, you can keep track of the “dangerous” days. However, due to fluctuations in hormone mucus may become viscous in the absence of ovulation, which makes the method inaccurate.
Lactation Amenorrhea Method
The point is simple: in the early months of breastfeeding ovulation does not occur, so we don’t have to protect ourselves. But there is a condition: a woman must breastfeed very actively (on-demand, or at least every three hours during the day and every six hours during the night) if the production of hormones prolactin and oxytocin is reduced – the “protective” effect disappears. However, too frequent feeding is not an absolute guarantee. The average duration of lactation amenorrhea is 4 to 8 months.
Spiral
IUD – a common and a rather simple method of contraception. This device is usually made of copper or silver with a plastic doctor installed in the uterus for several years. Copper or silver kills sperm, and the spiral itself, if fertilization does happen, prevents the egg to attach to the uterus (thus the embryo is not able to develop). The method is convenient because it requires almost no effort from women, but it has its shortcomings – for example, increases the risk of infections and inflammations.
Hormonal Contraception
Hormonal contraceptives there are many, and they act differently. In general, they can be divided into two types: those containing the hormones estrogen (or rather, their analogs) and those, which do not contain them.
Combined Hormonal Contraception
The most common method of hormonal contraception, if used properly, is one of the most reliable. Tablets contain two types of hormones, estrogens, and progestins. They suppress ovulation and pregnancy becomes impossible.
Surprising, but it is associated with fears most. Women are afraid of the side effects, such as blood clots: estrogens contribute to thrombus formation and increase the risk of thrombosis. In fact, this risk is much higher, during smoking or pregnancy. So if a woman has no serious contraindications (thrombosis history in a family, strongly elevated blood pressure, etc.), the use of spinners is considered safe. However, women are much more afraid of the overweight: the belief that the pill can lead to weight gain – is one of the most persistent. In fact, it is not true anymore: modern oral contraceptives contain a minimum dose of hormones, which, though they may slightly aggravate the feeling of hunger (but not necessarily), do not themselves increase the weight gain.
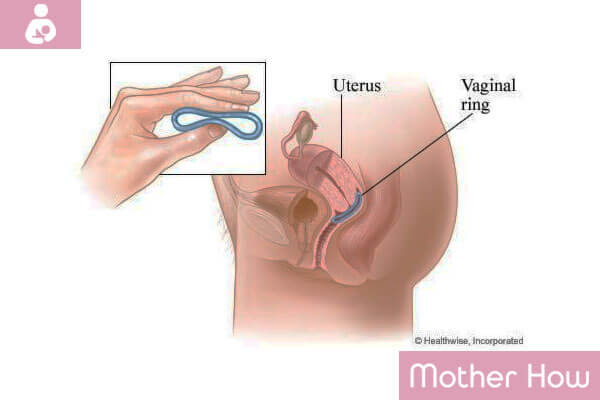
The Vaginal Ring
This is another method of hormonal contraception with estrogen. In terms of composition and principle of operation is similar to COCP but a radically different way of application. The flexible ring is inserted directly into the vagina, where the hormones that contribute to the suppression of ovulation are released in relevant doses. The advantage of the ring over COCP is that the ring gives almost no effect on the liver. A relative disadvantage is the application method: it may fall out of the vagina or interfere with a woman.
Hormone Patch
A hormone patch also contains estrogens, but sticks to the skin and delivers the hormones into the body through the bloodstream.
Mini-Pill
Another group of hormonal contraceptives, with no estrogen, but progestogen-only. Due to the absence of estrogen-related side effects, mim-pills are considered safer but less effective. This group includes the so-called mini-pill: a pill that contains a minimal dose of the hormone.
The principle of operation is different from estrogen-containing contraceptives: they do not prevent ovulation, but they cause thickening of the cervical mucus (mucus in the cervix), which prevents the sperm to penetrate the uterus itself.
Subcutaneous Implants
Particularly desperate women may decide to sew up a hormonal contraceptive implant under the skin, which also does not contain estrogen. It is set for several years and releases the hormone progestogen into the blood in the necessary quantity. Like a mini-pill, the implant increases the viscosity of cervical mucus and doesn’t allow the endometrium to swell.
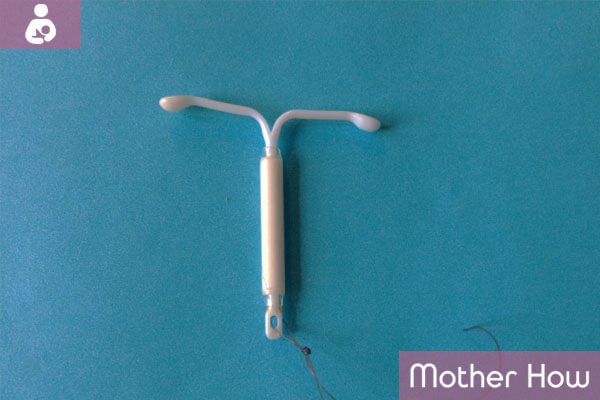
Hormonal IUD.
The operating principle is mixed. It immobilizes sperm and mechanically interferes with the embryo to attach to the uterus, just like the usual spiral. Furthermore, it allocates the minimum number of days the hormone progestin, which inhibits the growth of the endometrium and thus prevents the embryo to solidify.
Chemical Contraception
Vaginal suppositories, creams, foams, sponges, and tablets have spermicide effects, i.e. spermicides. Typically, these means should be used 10-15 minutes before the sexual intercourse. Their advantage is that they protect from diseases and sexually transmitted diseases – but not all of them and not fully. Disadvantage – the efficiency is much lower than that of other methods. Therefore, they are recommended to use in combination with other agents.
Emergency (Aka “Morning”) Contraception
If unprotected intercourse has already occurred, but a woman has no plans for a child, there is still something to do: for some time, you can still prevent conception with several methods.
Traditional Methods of Emergency Contraception
Slice of lemon, aspirin, soap, and a solution of potassium permanganate – not a complete list of funds that traditional medicine can offer to those careless lovers. It is understood that citric acid, a component of soap, potassium permanganate, and acetylsalicylic acid (aspirin), acidify the medium and kill sperm.
Doctors insist that those methods are strictly not recommended for two reasons. First – their low efficiency: the sperm can penetrate into the cervical canal a few seconds after ejaculation. And before that, it is, hardly possible to have time to put a lemon into the vagina. And the second – side effect: corrosive acids or improperly diluted potassium permanganate can “burn out” and disrupt the mucous vaginal microflora.
Hormone Pills
There is a more reliable method of postcoital (that is applied after sex) contraception. Special hormone pills. Though the containing substances are different from those of COCPs, the mechanism of action is similar: they suppress ovulation, and if conception has already occurred, do not allow a fertilized egg to attach to the uterine wall. Tablets are to be taken during the first few days after unprotected intercourse (the sooner, the better), but with each day of delay, their effectiveness will decrease.
It is widely believed that the use of such funds is extremely harmful, but the WHO has repeatedly stressed that they are safe. This obviously does not mean that such agents should be applied regularly they are simply not designed for this purpose.
Emergency Installation of a Spiral
The same spiral of copper or silver, mentioned above, can be set within five days after unprotected intercourse. The principle of work is the same: copper or silver detrimental effect on sperm and egg, and the spiral itself prevents the attachment of the embryo to the uterine wall. After the emergency installation, the spiral can be left inside as a permanent means of contraception.
Thus, we have listed all the known types of contraception. You may easily choose the right for you.

Born in Belarus, 1985, a pedagogue and family psychologist, mother. Taking part in procedures of social adaptation of the foster children in new families. Since 2015 is a chief editor of the motherhow.com project, selecting the best and up-to-date material for those, who are planning, expecting, and already having babies.

