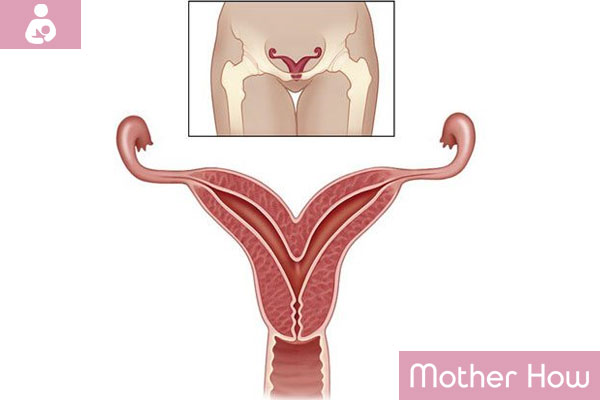
A bicornuate uterus (bicornate uterus) is an inborn abnormality of the uterus when it has two cavities. The bicornuate uterus is characterized by dysmenorrhea, abnormal uterine bleeding, violation of pregnancy, or infertility. Ultrasound, hysteroscopy, laparoscopy are used to diagnose. If necessary, endoscopic intervention is performed to restore the uterus (the Strassmann operation). Pregnancy and childbirth with the bicornuate uterus are possible, although it is associated with the increased risk.
Among the abnormalities of the uterus, the bicornuate uterus is the most common. But in general, it is diagnosed only in 0,1-0,5 % of women. The occurrence of the bicornuate uterus is connected with a violation of antenatal development.
If the bicornuate uterus is diagnosed, one cervix and one vagina are observed. But also, the doubling of the cervix is possible. One cavity of the bicornuate uterus may be rudimentary. In case the ovum is attached to the rudimentary cavity, pregnancy will be ectopic with the rupture of the cavity and peritoneal bleeding. In other cases, both cavities may be developed properly, and in both regular cycles with pregnancy and childbirth may take place.
What Causes a Bicornuate Uterus?
The formation of the bicornuate uterus may be caused by various factors that took place during the first months of pregnancy (the period of organs’ development). These include intoxication (alcohol, nicotine, drugs, chemicals) as well as vitamin deficiency, psychological stress during pregnancy, endocrine diseases (diabetes, hyperthyroidism), and heart diseases. Such infections as measles, rubella, influenza, toxoplasmosis, syphilis, and other diseases cause negative effects to the fetus. Chronic fetal hypoxia and toxicosis during pregnancy have negative effects as well. The bicornuate uterus may be accompanied by some other abnormalities like urinal system defects.
Bicornuate Uterus Symptoms
The presence of the bicornuate uterus may not be accompanied by clinical manifestations. Sometimes painful menstruation and uterine bleeding take place.
Often miscarriage or infertility may happen to women with a bicornuate uterus. But sometimes there are no problems during pregnancy and childbirth.
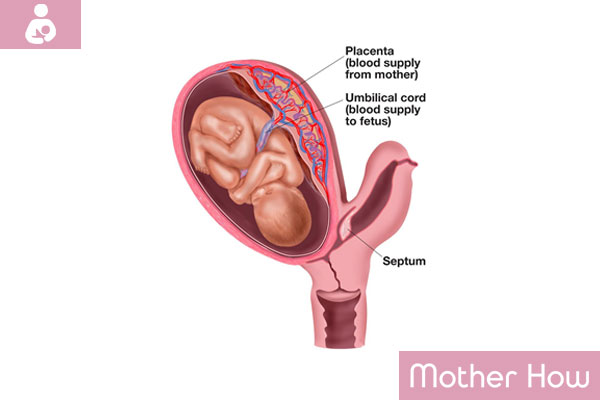
In cases of the bicornuate uterus, pregnancy usually takes place in one of the cavities, rarely in both. Pregnancy can be terminated in that case. That is why it is necessary to visit a specialist on a regular basis. Miscarriage usually happens during the first trimester. It may be caused by insufficient blood supply and the small size of the cavity.
Also, the abnormal position of the placenta may occur, it may cause placental abruption and bleeding. The presence of the bicornuate uterus increases the risk of cervical incompetence, premature childbirth, violation of the contractive muscles activity of the uterus, and postnatal bleeding.
How is a Bicornuate Uterus Diagnosed?
A bicornuate uterus may be suspected if the patient’s complaints – painful menstruation, abnormal bleeding, miscarriages, infertility – take place.
During the examination of the patient, the intubation of the uterus cavity is performed. It allows to figure out the shape of the uterus and find out if there is a bicornuate anatomical structure. A bicornuate uterus is detected during an ultrasound of the pelvis with the help of a vaginal or abdominal sensor.
Confirmation of the diagnosis is performed according to results of ultrasound, hysterosalpingography, MRI, hysteroscopy, laparoscopy.

Bicornuate Uterus Treatment
Surgery should be performed only in case of 2-3 miscarriages or in the case of infertility. The surgery is aimed at restoration of the uterus with one cavity. More often the removal of the rudimentary cavity takes place (Strassman, Thomson operations).
Strassman surgery is a standard procedure. Basically, it is a laparotomy. Also, the surgery may be performed with the help of a hysteroscopy. After surgery, an intrauterine device should be used for at least 6-8 months.
Prognosis
With sufficient capacity of the uterine cavity, pregnancy goes without complications. In severe cases, there is a high risk of miscarriage or premature birth.
Pregnancy in women with a bicornuate uterus requires prevention of miscarriage, development of cervical incompetence, bleeding. When there is a risk of pregnancy termination in the later stages (after 26-28 weeks of pregnancy), a cesarean section is performed in order to save the fetus.
In the case of a full-term pregnancy, delivery depends on various factors (for example, the position of the fetus).
After the surgical intervention, the risk of miscarriage in women with a bicornuate uterus is reduced from 90% to 30%.

Born in Belarus, 1985, a pedagogue and family psychologist, mother. Taking part in procedures of social adaptation of the foster children in new families. Since 2015 is a chief editor of the motherhow.com project, selecting the best and up-to-date material for those, who are planning, expecting, and already having babies.