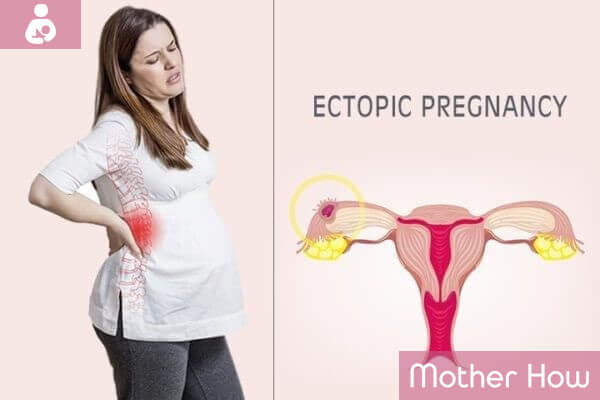
In order to develop the pregnancy in a normal and safe way for the mother’s body the fertilized ovum (embryo) must get into the uterine cavity via fallopian tubes and penetrate into the endometrium.
In the case of ectopic pregnancy, the embryo does not get into the uterine cavity, and attaches and begins to grow elsewhere. Most often, ectopic pregnancy develops in the fallopian tubes, on the ovaries, in the cervix, or on the intestines.
With the development of the embryo, the organ to which it was attached is destroyed; it can cause severe internal bleeding, life-threatening to a pregnant woman.
Normal development of pregnancy is possible only within the uterine cavity. In the case of ectopic pregnancy, the embryo attaches outside the uterine cavity, for example, in a fallopian tube.
Ectopic pregnancy is a very dangerous state and it’s one of the main causes of death of pregnant women in the first trimester of pregnancy.
Before the invention of modern techniques of anesthesia and operations, as well as before the discovery of antibiotics and blood transfusion, only 1 of 6 women with ectopic pregnancies survived.
Despite the fact that, as in earlier times, ectopic pregnancy accounts for about 2% of all pregnancies, now, thanks to the timely intervention of doctors, it rarely ends with the death of a pregnant woman.

Causes of Ectopic Pregnancy
The cause of ectopic pregnancy can be a variety of diseases or conditions that interfere with the normal movement of the fertilized egg in the fallopian tubes into the uterine cavity.
The most common causes of ectopic pregnancy are sexually transmitted infections (chlamydia, gonorrhea, trichomoniasis). These infections cause inflammation of the fallopian tubes, narrowing, and deformation of their lumen, which finally can cause “stopping” of the embryo in the fallopian tube. Being stopped, the embryo begins to grow, and very soon it destroys the fallopian tube.
In the case of chlamydia, or trichomoniasis (rarely in the case of gonorrhea), ectopic pregnancy may be the first manifestation of infection because very often, these diseases are not shown by any other symptoms.
For some women, the cause of an ectopic pregnancy can be the operation performed on the fallopian tubes or other internal organs, as well as tubal ligation for the purpose of sterilization or treatment of infertility with medicines (clomiphene, gonadotropin preparations). See also infertility and its treatment.
According to research reports the risk of ectopic pregnancy:
- Increased for 1.5-2 times for women using the intrauterine device
- For 3-4 times among women aged 35-45 years
- For 3.5 times for women who smoke
Quite often, for unknown reasons, an ectopic pregnancy occurs in completely healthy women who have no factors of risk and no illnesses from those that were described above.
The risk of a recurrence of ectopic pregnancy among women who in the past had an ectopic pregnancy is about 25%.
Symptoms and Signs of Ectopic Pregnancy
Symptoms and signs of ectopic pregnancy depend on its duration. For a period of 1-2 weeks, ectopic pregnancy can’t be shown.
Later, at 3-4 weeks there may be signs of a normal pregnancy.
- Increased basal body temperature
- The long delay of menstruation
- Nausea
- Voltage and sensitivity of a breast
A detailed description and explanation of all the possible signs of pregnancy are presented in the article Signs of pregnancy.
Suspected ectopic pregnancy should appear if in addition to the normal signs of pregnancy there are symptoms such as:
- Acute or nagging, dull pain in lower abdomen (perhaps on the right or on the left)
- Blood leakage from vagina, not like menstruation
- Pain during sexual intercourse
For a period from 4 to 20 weeks, an ectopic pregnancy can rupture the fallopian tube (or another organ to which it was attached), and severe bleeding. The first symptoms of these complications may be:
- A strong, piercing pain in the abdomen
- Sudden weakness, loss of consciousness, paleness, rapid pulse
- Blood leakage from a vagina
Consequences and Complications of an Ectopic Pregnancy
The most dangerous complication of ectopic pregnancy is strong internal bleeding, caused by the rupture, which can be lethal for a pregnant woman in several tens of minutes or hours.
Other possible consequences of ectopic pregnancy are a repeat of ectopic pregnancy after a while, or the development of infertility because of the destruction of the fallopian tubes.
Because of the fact that in some cases an ectopic pregnancy develops in the organs with rich blood supply (ovaries, place of transition of the fallopian tubes into the uterus) surgery of removal of the ectopic pregnancy can end as removal of a fallopian tube, removal of the uterus with both fallopian tubes or the removal of one of the ovaries.
Ectopic pregnancy reduces the chances of a woman conceiving a child in the future, however, if during surgery the doctors are able to save the uterus and ovaries, the ability to conceive a child remains (see Infertility treatment).

Tests and Inspection
To detect an ectopic pregnancy, the following analyzes and inspections are taken place:
Pelvic Ultrasound (of Uterus and Uterine Appendages)
Ultrasound helps to identify an ectopic pregnancy at the end of the first month of its development. Transvaginal (through the vagina) ultrasound can detect ectopic pregnancy approximately in 4 weeks, and transabdominal (through the abdomen) ultrasound in 5 weeks. A detailed description of how does pelvic ultrasound is held, how to prepare for the procedure, and what might mean its terms of the results is reported in the article: A pelvic ultrasound.
Identify The Level of Human Chorionic Gonadotropin (HCG) in the Blood
This analysis helps to reveal the fact of pregnancy and to suspect ectopic pregnancy if the concentration of HCG in the blood of pregnant women increases more slowly than it does in normal pregnancy. See also What may mean the results of analysis on HCG?
A Home Pregnancy Test
As with a normal pregnancy, ectopic pregnancy, home pregnancy tests show positive results. Due to the fact that the home test is less sensitive than the laboratory tests for HCG and also because they don’t determine the concentration of HCG in the blood, but only show its presence – they can’t be used to determine accurately the ectopic pregnancy.
Important!
In all cases, when a home pregnancy test shows a positive result it’s necessary to visit a doctor as soon as possible for a pelvic ultrasound, which will allow identifying in time an ectopic pregnancy (see. How to do a home pregnancy test?).
Laparoscopy
This survey is conducted in the case when doctors suspect a woman has internal bleeding, developed on the background of an ectopic pregnancy. The main symptoms of internal bleeding are severe abdominal pain, sudden weakness, pale skin, and loss of consciousness.
Laparoscopy is performed under general anesthesia and involves investigation of the pelvic organs (in particular: uterus, fallopian tubes, and ovaries) using a special video camera inserted into the abdomen through a small hole, which heals quickly after surgery.
Laparoscopy allows distinguishing an ectopic pregnancy from ovarian cysts or endometriosis, which can be manifested with similar symptoms. If in the course of laparoscopic diagnosis of ectopic pregnancy is confirmed, the survey becomes into medical operation, during which doctors remove the embryo attached incorrectly and stop the bleeding.
A detailed explanation of how does laparoscopy performed and how passes the recovery from this operation is presented in the article Laparoscopy.
The Treatment of Ectopic Pregnancy
In the case of an ectopic pregnancy is not possible to save the child’s life, so the sole purpose of treatment is to save the life of a pregnant woman.
Treatment Without Surgery
Treatment of an ectopic pregnancy without surgery (conservative treatment), however, may be carried out relatively rarely and only in cases when the size of the embryo does not exceed 3.5 cm and a woman can be kept under the supervision of a doctor, who at the first need will make an operation.
The treatment is carried out with the medicine methotrexate, which stops the development of the fetus and leads to its rejection.
There are possible side effects of methotrexate treatment of ectopic pregnancy: nausea, vomiting, diarrhea, pain in the upper abdomen, a temporary increase in ALT and AST in blood. In rare cases, there are temporary hair loss and the appearance of serious complications of the heart, lung, and bone marrow.
Important!
The treatment of ectopic pregnancy with methotrexate is contraindicated in case of:
- Women who breastfeed
- Women with lowered immunity (for example, diabetic patients)
- Women suffering from liver disease, diseases of kidney, stomach or blood
During treatment with methotrexate it’s prohibited:
- To consume alcoholic drinks
- To take multivitamins or folic acid or anti-inflammatory drugs such as ibuprofen or aspirin
- To have sexual contacts
In some cases, treatment with methotrexate does not give the desired result and an ectopic pregnancy continues to develop. In this regard, a few days after taking methotrexate it’s necessary to turn again to the doctor to assess the effectiveness of treatment. Ask your doctor obligatorily about the time of the second visit and in any case, don’t miss it.
The Operation for the Treatment of Ectopic Pregnancy
A surgical treatment (an operation) is the most reliable method of treatment of ectopic pregnancy. Currently, laparoscopic operations are used often, during which the embryo is removed through small openings in the abdomen of the patient.
A usual operation with the cut of the abdomen (laparotomy) is performed in cases when ectopic pregnancy is complicated by severe bleeding or is out of reach for laparoscopy (for ex., cervix, bowel).
In cases when women don’t want to have children or women with repeated ectopic pregnancy in the same fallopian tube, the doctors can recommend the complete removal of the fallopian tubes to prevent the recurrence of ectopic pregnancy in the future.
Recovery after an operation concerning an ectopic pregnancy usually goes quickly (especially in the case of laparoscopic surgery). Wounds after operation heal completely for 2-3 weeks.
During 2-3 months after surgery, it’s necessary to avoid physical exertion and constipation (see Effective treatment of constipation for adults).
After the operation or conservative treatment, the doctor may ask you some more time to be tested for HCG (HCG levels are usually monitored up to 0). This is necessary in order to make sure that after surgery there are no fragments of membranes in your body that continue to grow and may eventually turn into a tumor.

Born in Belarus, 1985, a pedagogue and family psychologist, mother. Taking part in procedures of social adaptation of the foster children in new families. Since 2015 is a chief editor of the motherhow.com project, selecting the best and up-to-date material for those, who are planning, expecting, and already having babies.